
Postural Orthostatic Tachycardia Syndrome

What is POTS?
Postural Orthostatic Tachycardia Syndrome (POTS) is one of the most common forms of dysautonomia. It affects how the autonomic nervous system regulates heart rate and blood flow.
People with POTS experience an abnormally large increase in heart rate when moving from lying down to standing by 30 beats per minute in adults (40 bpm in teenagers), without a significant drop in blood pressure. This rapid heart rate can cause dizziness, light-headedness, or even fainting. POTS is a condition that affects daily life but is often misunderstood or overlooked.
Common Symptoms
Symptoms vary from person to person, but may include:
Rapid heartbeat or palpitations
Dizziness or fainting when standing
Fatigue and exhaustion
Brain fog and difficulty concentrating
Nausea or stomach upset
Headaches and blurred vision
Difficulty regulating body temperature
Shakiness or tremors
POTS symptoms often worsen with heat, illness, dehydration, stress, or long periods of standing.
Diagnosis
POTS is diagnosed by doing an active stand test measuring heart rate and blood pressure every couple of minutes
Diagnostic criteria
Symptoms of orthostatic intolerance lasting >3 months
Sustained increase* of more than 30 bpm (>40 for 12-19 years)
No sustained drop in blood pressure >20/10 mmHg withing the first 3 minutes of standing
Exclusion of other causes of symptoms
*sustained increased is defined as two measurements made at least one minute apart
Postural Orthostatic Tachycardia Syndrome

Management strategies
There is no single cure for POTS, but symptoms can often be improved with lifestyle changes and, in some cases, medication.
Lifestyle strategies may include
Drinking 2–3 litres of water daily
Increasing salt intake (if medically safe)
Wearing compression stockings to support circulation
Eating smaller, more frequent meals
Avoiding prolonged standing and overheating
Building tolerance with gentle, recumbent or seated exercise including resistance training.
Medical treatment may also be needed and may involve medications to manage blood pressure, heart rate, or blood volume- always guided by a medical specialist.
Orthostatic Hypotension
What is Orthostatic Hypotension?
Orthostatic Hypotension (OH) occurs when blood pressure drops significantly upon standing, leading to dizziness, light-headedness, or fainting. It is often a result of the autonomic nervous system not responding appropriately to changes in posture.
Common Symptoms
Symptoms vary from person to person, but may include:
Light-headedness or dizziness when standing
Fainting (syncope)
Fatigue or weakness
Blurred vision or “tunnel vision”
Nausea
Palpitations
Diagnosis
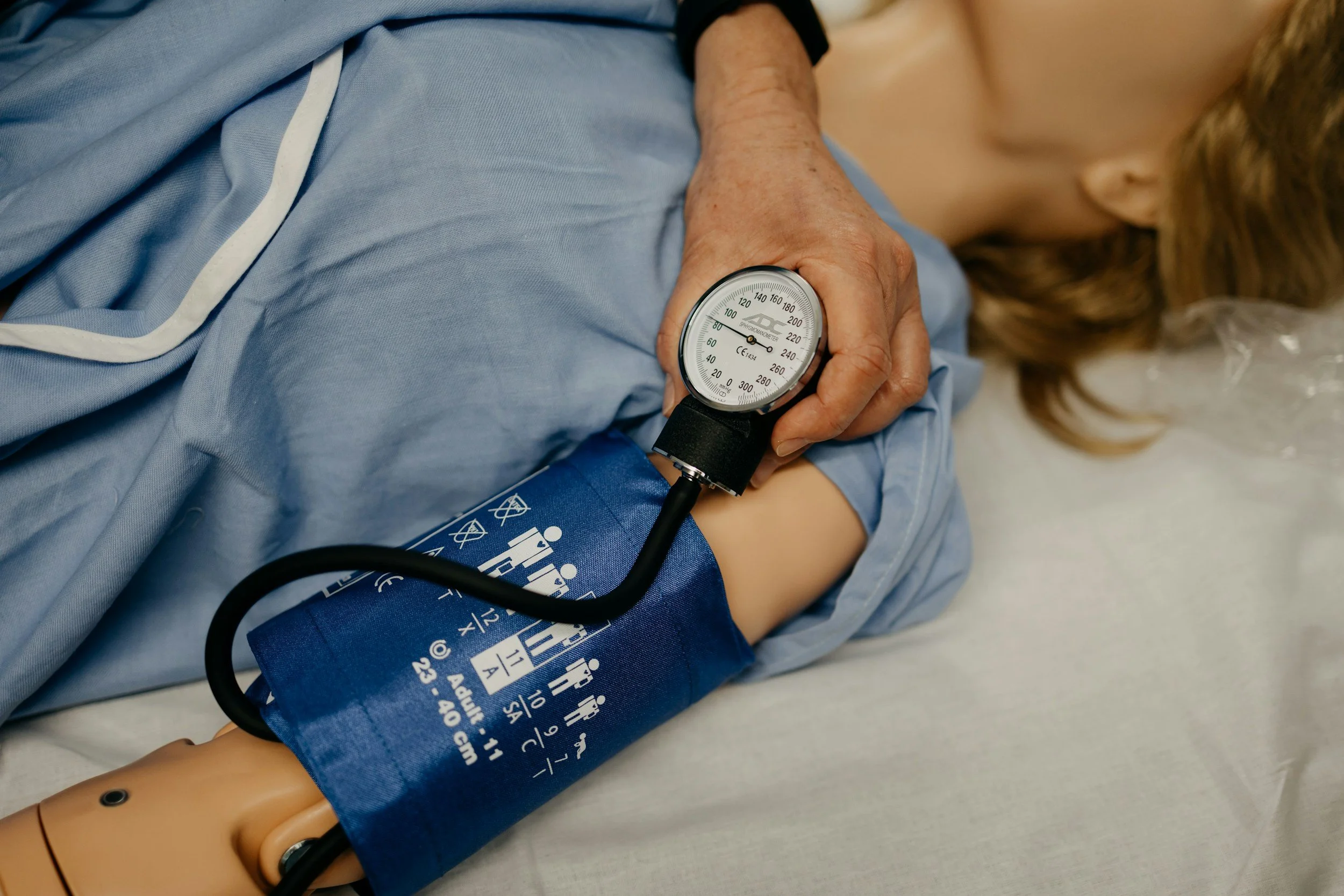
Blood pressure measurements while lying down, sitting, and standing done by a medical professional. Active Stand Test is used to confirm the drop in blood pressure
Management strategies
Management strategies should be discussed with a medical professional but other lifestyle strategies similar to POTS can be effective.
Inappropriate Sinus Tachycardia


What is Inappropriate Sinus Tachycardia
Inappropriate Sinus Tachycardia (IST) is a condition where the heart beats faster than normal at rest or with minimal activity, without an underlying cause such as fever, dehydration, or other medical conditions. The fast heart rate arises from abnormal regulation of the sinus node, the heart’s natural pacemaker.
Common Symptoms
Persistent or rapid resting heart rate (often >100 bpm)
Palpitations or awareness of the heartbeat
Fatigue and exercise intolerance
Dizziness or light-headedness
Shortness of breath
Anxiety or feelings of “racing heart”
Diagnosis
Electrocardiogram (ECG) to monitor heart rhythm
Holter monitor or event monitor to track heart rate over time
Exclusion of other causes of rapid heart rate (thyroid issues, anemia, medications etc.)
Management Strategies
Lifestyle modifications: pacing activity, managing stress, and avoiding stimulants (caffeine, certain medications)
Exercise programs: gentle, structured cardiovascular activity to improve tolerance
Medications: beta-blockers or other heart-rate controlling drugs may be prescribed under specialist supervision
Monitoring & Support: ongoing assessment by a cardiologist or autonomic specialist is often recommended
Useful Recourses

Dysautonomia International
A leading nonprofit providing research updates, patient education, clinician resources, and conference materials.
Includes patient guides and expert insights on POTS and broader autonomic disorders.
🔗 https://dysautonomiainternational.org
Dysautonomia Information Network (DINET)
A comprehensive site focused on dysautonomia (including POTS) with explanations, research summaries, and forum links.
🔗 https://www.dinet.org
The Dysautonomia Project
Curated resources for both clinicians and patients, including education modules and a clinician course.
🔗 https://thedysautonomiaproject.org
Australian POTS Foundation
Offers current clinical summaries, consensus statements, and state-of-the-science reviews (including 2026 updates).
🔗 https://potsfoundation.org.au
